We were approached by one of the largest insurance companies in the Northwest, providing coverage to over 2 million people across Washington and Alaska. Their goal was to reimagine the customer experience (CX) for its users centering around the member portal.
Health Plan Provider
Reimagining the Key Moments of a Patient’s Journey for the Largest Health Plan Provider in the Pacific Northwest
Opportunity
Project Info
CLIENT
Health Plan Provider
services
Ideation/Envisioning,Prototyping, Journey Mapping, Digital Strategy, Visual Design, UX Design
Type
Web Portal
Heeding the Call
Our client brought this envisioning problem to UpTop because they were in need of an outside-in perspective. The CX and Innovation teams at the health insurance company had accumulated some great customer research and were ready to take action on these valuable insights.
UpTop recognized that the client team needed to expand their vision for this project, and utilize a more ‘10x thinking’ approach. Like others in the healthcare industry, they have been constrained by legacy systems that inhibit the technological innovation and design vision that many other companies get to experience more easily.
UpTop recognized that the client team needed to expand their vision for this project, and utilize a more ‘10x thinking’ approach. Like others in the healthcare industry, they have been constrained by legacy systems that inhibit the technological innovation and design vision that many other companies get to experience more easily.
challenge
The existing Member Portal relied on many 3rd-party solutions, some of which could potentially be built in-house to gain control over the customer experience.
solution
A multi-day envisioning workshop, with journey mapping at the core, helped the large group of stakeholders align and empathize with the members’ experience.
outcomes
A carefully crafted story and prototype reimagined key moments of a patient’s journey, effectively through new self-service experiences, aimed at reducing support call volumes.

“I am very pleased with the outcome and I’m looking forward to sharing this work internally with our business partners.”— Director of Product Management & CX
Our Approach
We meticulously planned a multi-day envisioning workshop, with design thinking and ideation activities for client's CX team, and key constituents. UpTop’s goal was to align the interests of all parties involved so they could work to define a successful future for the Portal.
The workshops enabled cross-functional collaboration, and created a shared vision of the customer journey. Journey maps of each flow (Shop & Enroll, Find Care, Benefits, Pharmacy, and Claims) were documented and reviewed with the group. This allowed all the participants to better understand the specific workflows and subject matter experts to discuss key areas of friction as well as provide context for decisions that made up the experience.
Being able to share openly in the workshop setting helped leaders of the different groups gain alignment. The Director of Product Management and CX was empowered to let the team know there was no longer a mandate to use legacy systems.
The ideation activities allowed the team to stretch their thinking beyond what they were used to – breaking through the institutional walls and absent the fear of rejection that may come within them.
The workshops enabled cross-functional collaboration, and created a shared vision of the customer journey. Journey maps of each flow (Shop & Enroll, Find Care, Benefits, Pharmacy, and Claims) were documented and reviewed with the group. This allowed all the participants to better understand the specific workflows and subject matter experts to discuss key areas of friction as well as provide context for decisions that made up the experience.
Being able to share openly in the workshop setting helped leaders of the different groups gain alignment. The Director of Product Management and CX was empowered to let the team know there was no longer a mandate to use legacy systems.
The ideation activities allowed the team to stretch their thinking beyond what they were used to – breaking through the institutional walls and absent the fear of rejection that may come within them.
Outcomes
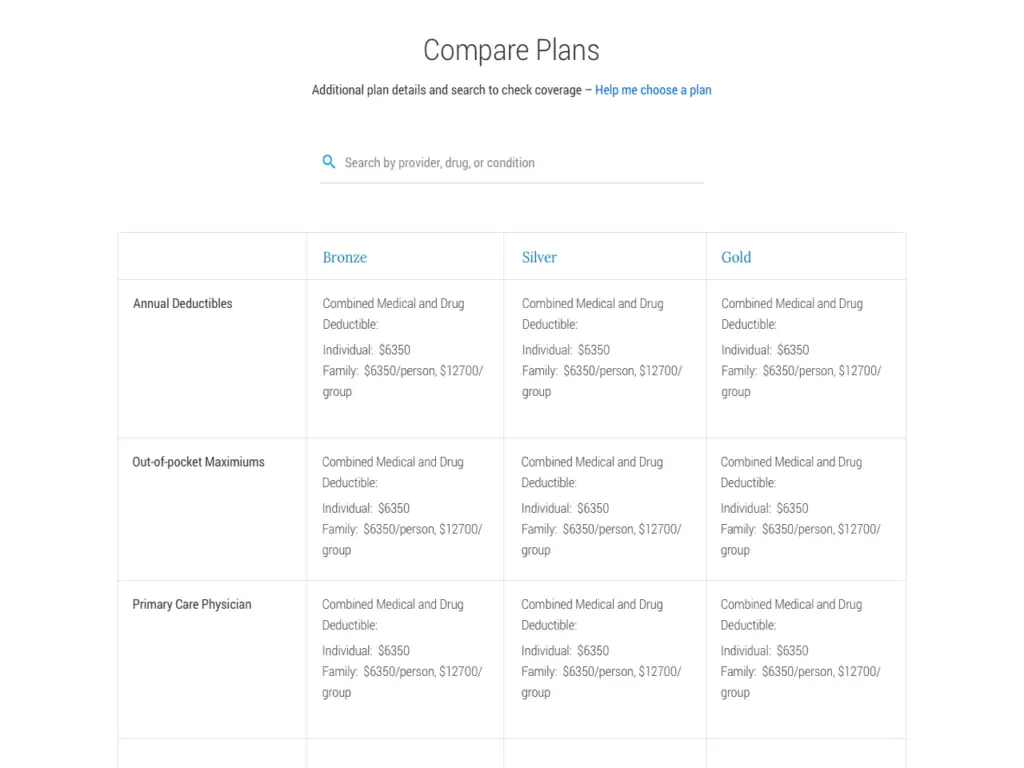
The common thread that wove the main pillars of Shop & Enroll, Find Care, Benefits, Pharmacy, and Claims together was achieved through an elaborate user story of a fictitious person and her interactions of key moments within the new member portal. This prototyped experience of ‘Mary’s journey’ allowed us to cover each stakeholder group and reimagine experiences throughout the portal, effectively creating new self-service experiences, which would result in a major reduction of support call volumes.
Areas of Focus
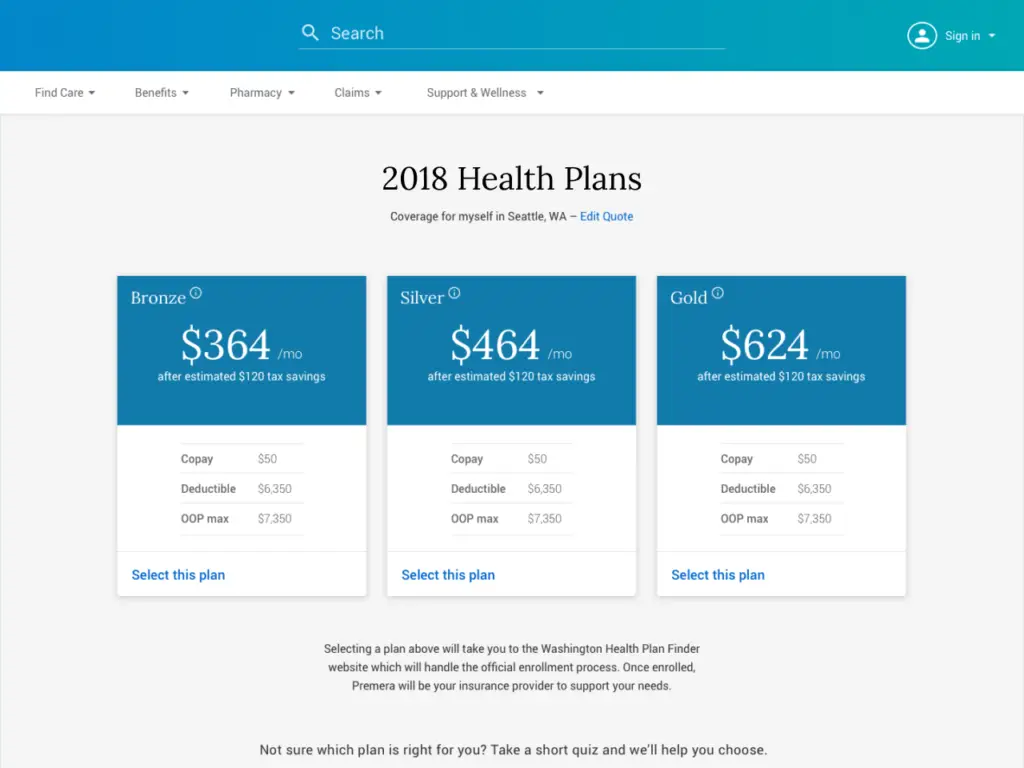
- Simplified the shop & enroll experience of healthcare plans for new customers
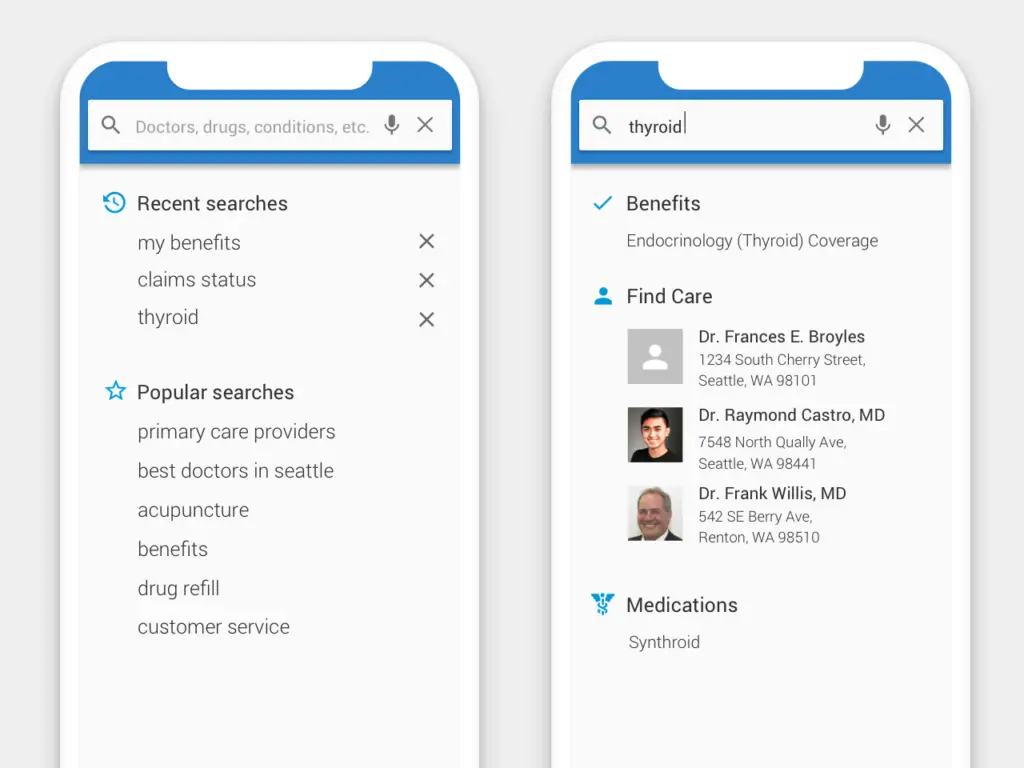
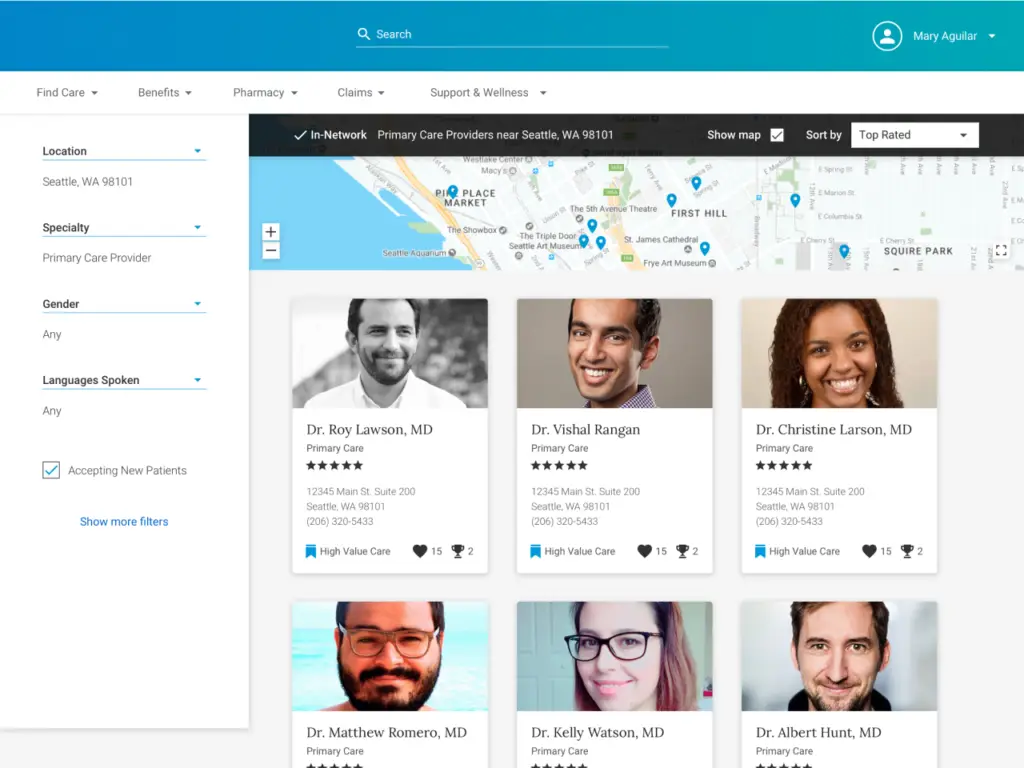
- Streamlined the search experience for how members find the care that they need
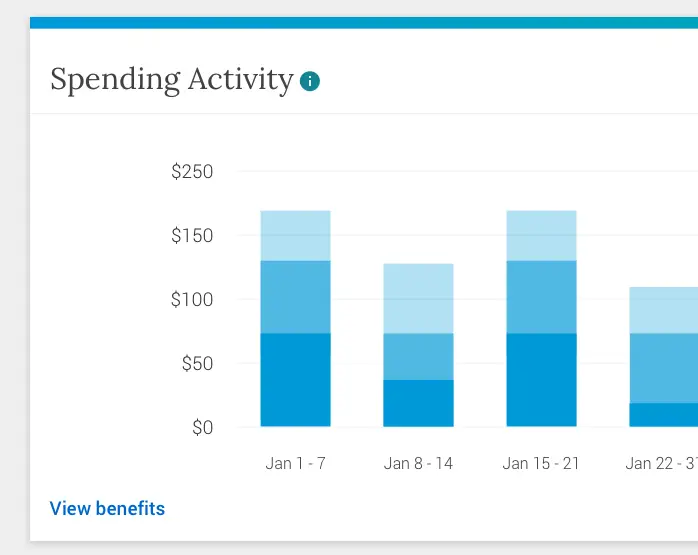
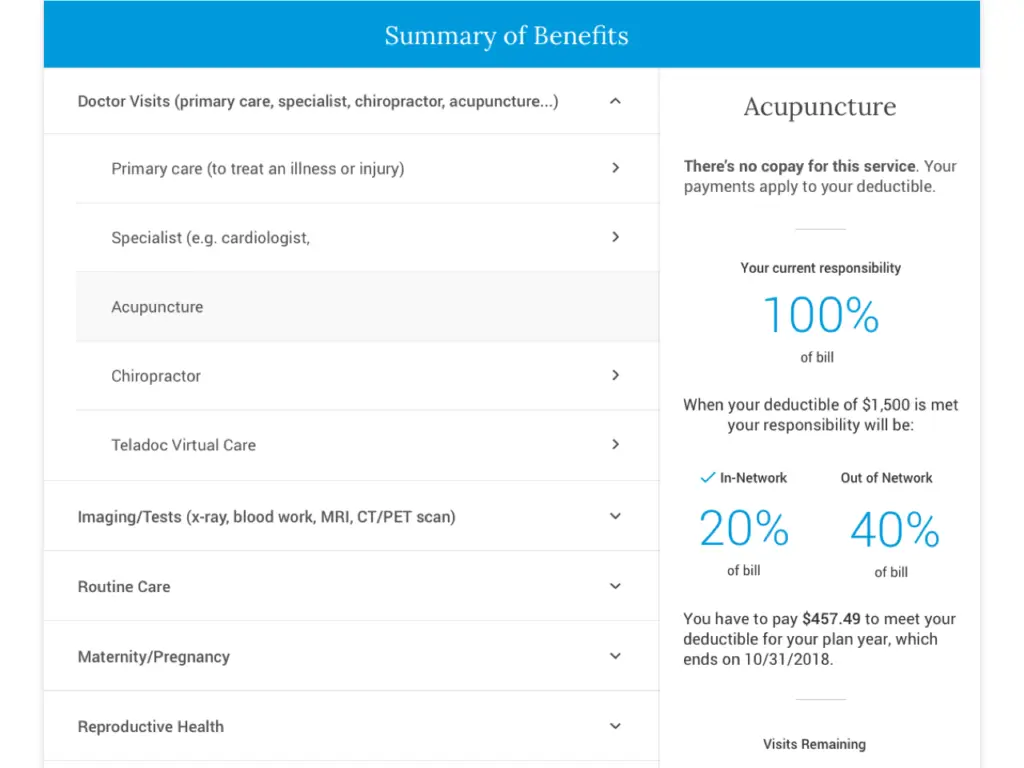
- Synthesized member benefit information in strategic locations within the portal
- Integrated third-party pharmacy data within the portal and allowing members to refill prescriptions
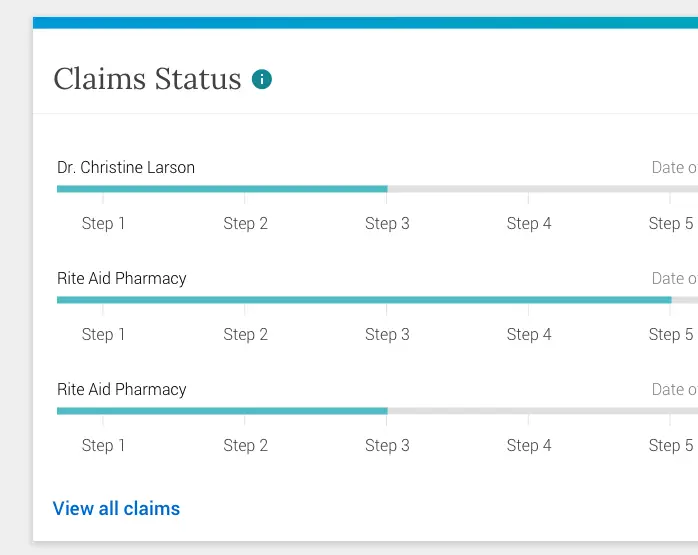
- Optimized the ability to submit a claim effortlessly and view claim statuses
More Projects
Engaging Inside Sales Millennials with Microsoft
F5
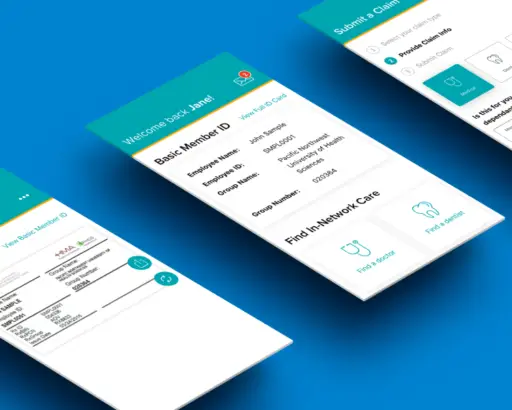
HMA (Healthcare Management Administrators)

The L.A.U.G.H. TIME Program
JAMS
OYO
Los Alamos National Laboratory
Mattress Firm

Pearson Packaging HMI
Belkin’s Linksys Velop Mobile App
Starting children’s day with art, calmness, and The L.A.U.G.H. App

Southwest Airlines
VUDU Windows 10 Universal App
Diptic Photo Editing App

Ambient Art®
Microsoft Partner Network Portal
BusMe
Vimocity

Ready Hawaii Mobile App
Let's make awesome things, together.
Whether you are looking to create a new product or update an old design, we are here to assist you.